 All recruited patients received detailed ophthalmological examination that included slit-lamp anterior segment examination, intra-ocular pressure (IOP) measurement using applanation tonometry, slit-lamp biomicroscopy to determine the presence of a macular hole and associated features of high myopia including posterior staphyloma and chorioretinal atrophic patches, and indirect ophthalmoscopy with 360-degree scleral indentation to exclude the presence of peripheral retinal breaks. In addition, the study excluded patients with recurrent retinal detachment after previous scleral buckle surgery or PPV, patients presenting with proliferative vitreoretinopathy grade C, patients with macular disease that would compromise the final best-corrected visual acuity (BCVA) as myopic choroidal neovascular membrane, recruited patients who did not present for silicone oil removal after initial surgery, patients who did not complete at least 3 years of follow-up after silicone oil removal, and patients with dense media opacity, including cataracts, that precluded adequate pre-operative assessment of the macular hole or the retinal periphery. Exclusion criteria included patients presenting with retinal detachment attributed to pathologies other than high myopia as rhegmatogenous retinal detachment with peripheral breaks, trauma, tractional diabetic disease, or congenital disease as optic pit maculopathy. The study exclusively recruited patients with high myopia whose axial length measured ≥26 mm and had associated retinal detachment secondary to the macular hole. The study included patients with MRDMH operated on between 20 in a tertiary retina center Magrabi eye hospital, Tanta, Egypt. This is a retrospective interventional non-comparative consecutive case series. 18–20 In the present study we used PPV and silicone oil tamponade for management of MRDMH and focused on exploring the anatomical and functional outcomes of this technique and its long-term validity after silicone oil removal. 
To date, the timing of silicone oil removal is still debated. 2, 7, 9, 13–17 Nevertheless, the issue of using silicone oil mandated defining the appropriate time for its removal to avoid a recurrence of retinal detachment and to avoid silicone-oil induced complications particularly secondary glaucoma. Finally, silicone oil defers prone positioning of the patient that would be otherwise required for a long period of time and entails non-compliance of the patient. Secondly, silicone oil tamponade provides protracted tamponade duration that would increase the odds of retinal re-attachment in the presence of underlying atrophic RPE and choroid by providing a scaffold to stimulate glial proliferation across the hole and allowing time latitude for absorption of sub-retinal fluid. Overstretch is produced by forcible backward displacement of the retina by the gas bubble with possible enlargement of the hole or compromise of the centripetal movement of photoreceptors to close the hole, subsequently resulting in higher incidence of open macular hole or even iatrogenic enlargement of the hole. Firstly, silicone oil provides the desired tamponade effect while averting centrifugal overstretch of the inelastic retina around the hole. 6–12 Some authors advocated that a longer term tamponade provided by silicone oil could improve the surgical outcome of MRDMH patients for several reasons. 2–5 Hence, several alternative techniques were introduced for MRDMH, though with no consensus to date among retina surgeons on one optimal surgical approach.  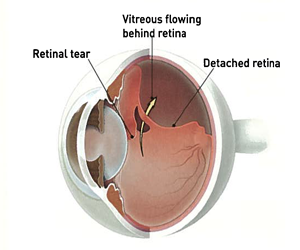
The subsequent inability of the inelastic retina to conform to the concavity of the staphyloma and poor adhesion between the neurosensory retina and the underlying atrophic retinal pigment epithelium (RPE) and choroid were major causes of failure. 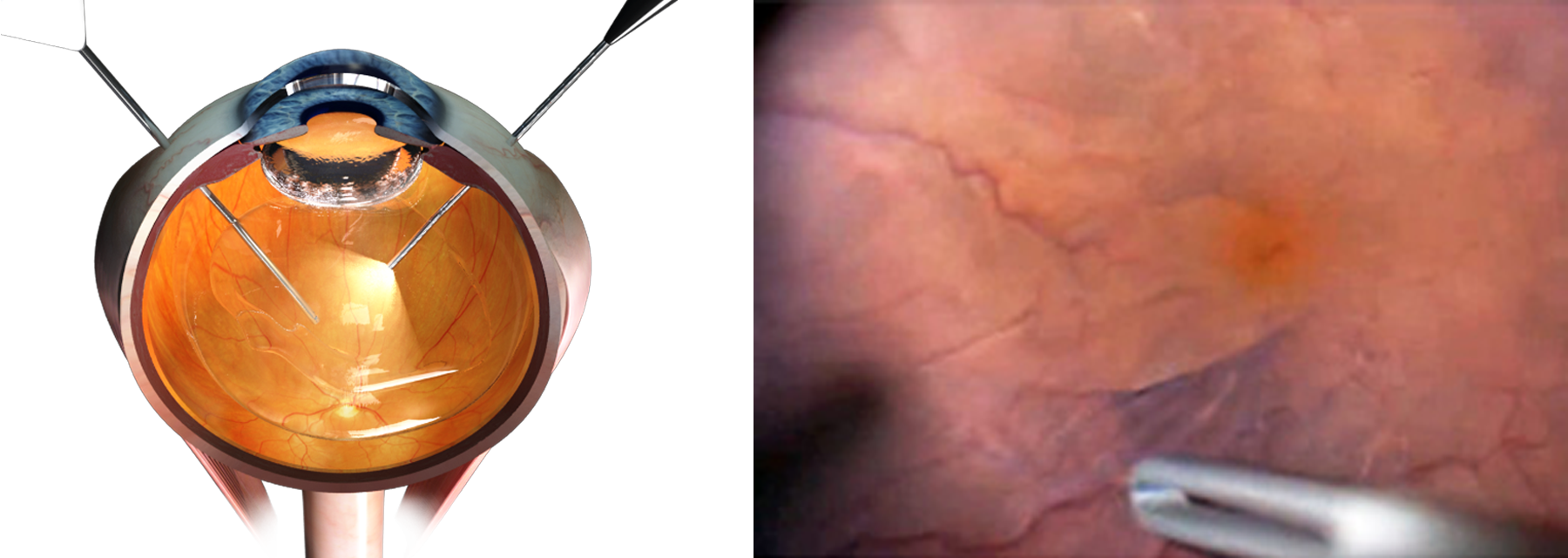
A plausible explanation is that the technique of Gonvers and Machemer focused on relieving the anteroposterior traction force in the posterior pole rather than addressing the multifactorial etiology of MRDMH, particularly in the subgroup of patients with posterior staphyloma and extensive chorioretinal atrophy. 1 However, several studies using this technique reported variable success rates with considerable discrepancy among authors regarding the validity of the technique to achieve retinal re-attachment and macular hole closure. Gonvers and Machemer in 1982 introduced pars plana vitrectomy (PPV) and partial gas-fluid exchange for management of MRDMH. Surgical management of myopic retinal detachment associated with macular hole (MRDMH) is an existing dilemma. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
